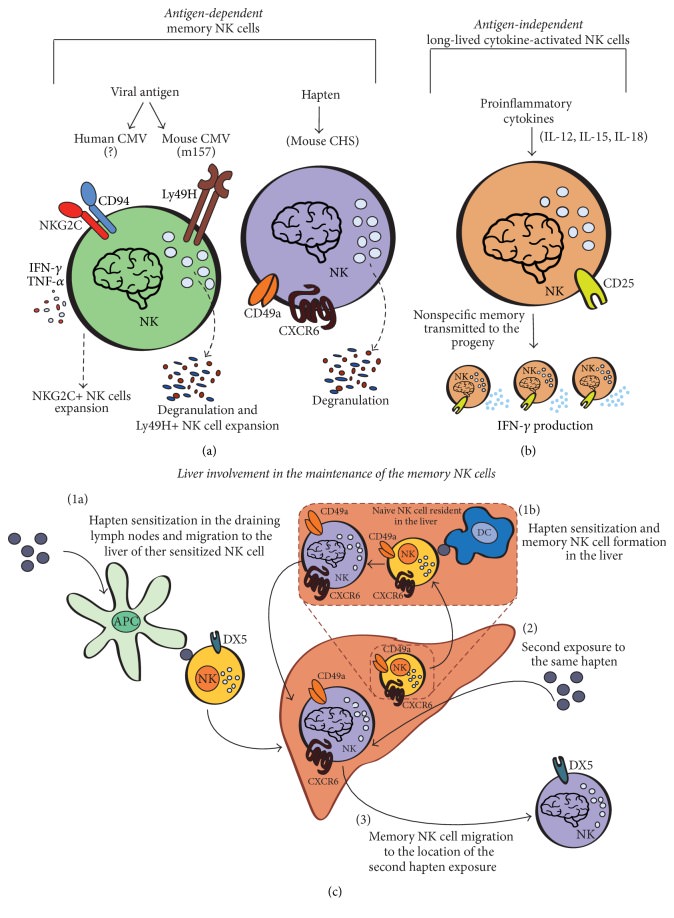
Many of
my chemically sensitive clients have reactions from inhaling, eating, and
skin/air contact with chemicals.
Haptens' effect
on the immune system supports why they can wear a gas mask in a perfumey room and still get sick.
I
haven't seen anyone else online talking about haptens
and I've noticed that a lot of my allergies and chemical sensitivities have
improved by reducing my hapten exposure.
In
study models, haptens can be used in to induce food
intolerance, chemical sensitivities, skin disease, and autoimmunity.
In this
post, we will discuss the how haptens may have
detrimental effects in humans.
Too Long, Didn't Read (TLDR):
·
Haptens can
activate the immune system spontaneously (without a carrier protein) or via
Cross-linkage (needs a carrier protein such as proteins, lipoproteins,
polysaccharides or other large molecules in order to become antigenic). R R
·
Haptens are
inhaled, ingested, or come into contact with the skin. R
·
Once the body has generated antibodies to a hapten-carrier
adduct, haptens themselves may bind to the antibody,
creating an immune response. R
·
Multiple haptens may cluster together
and create a bigger antibody response (this is useful for vaccines, but may put
those with hapten sensitivity on overload) R
·
Haptens may
drive autoimmunity with their ability to create antibodies R R R
·
For example, haptens can bind to tight
junction proteins creating antibodies against them and may cause intestinal
permeability while also binding to LPS making
neuroinflammation and endotoxemia worse. R R R
·
Being Th17 dominant (having high IL-17 or IL-25 levels)
increases symptoms to hapten sensitivity R R
·
They modify lectin and mannose binding R
·
Haptens have
the ability to induce chemical sensitivities, atopic dermatitis
(eczema), GI problems (food intolerance and allergy), urticaria
(via mast cells), anemia,
CNS changes (such as hyperactivity), alcohol intolerance
R R
·
Haptens either
work in the skin and give you skin disease or work internally and give you
autoimmune like conditions, but typically not both (patients with atopic
dermatitis have heightened oral tolerance to dietary haptens)
R
·
Short term, lower doses of haptens may
not cause any problems, BUT long term or high dose hapten
exposure may cause sensitization and immune problems. R R
·
Some essential oils have prehaptens that autoxidize (oxidize from air
exposure) that then turn into haptens
·
It is still not known why we react to some haptens
and not others.
What Are Haptens?
The
term hapten is derived from the Greek haptein, meaning “to fasten".
A hapten is any chemical that have a molecular weight lower
than 1 kDA (<1000 Daltons).
Haptens were
not very common until the past hundred years when we started to manufacture and
create our own chemicals (a new environment with man-made things).
There
is a high correlation between haptens in the
environment and the rise in new allergies. R R
Common
belief is that since haptens are so small, they do
not directly induce antibody response and need to bind to a large protein (some
examples of conjugated proteins are via serum globulin, albumins, ovalbumin,
poly-L-glutamic acid, polysaccharides and liposomes). R R
On top
of that, once the immune system is primed for a class of haptens,
it no longer needs the carrier proteins for haptens
to bind as an antigen.
Some
studies have shown there are exceptions, and thus haptens
may activate the immune system without the need for a larger carrier
protein. R
Methods Of Hapten
Conjugation (Haptenization):
·
Intermediary Molecules Cross-linkage -
mainly applies to nonreactive haptens and dependent
on the right environment (such as 1. carbodiimide or 2. glutaraldehyde - Schiff
bases or Michael-type double bond addition products) R
·
Spontaneous Chemical Reaction - no
cross-linking agents are needed R
|
Common |
Mediator |
Antigen |
Effector |
Example |
|
|
Type I |
Immediate |
IgE |
Soluble |
Mast Cell |
Peanut Anaphylaxis |
|
Type II |
Bystander |
IgG Monomer |
Cell or Matrix |
Complement, |
PCN-assoc. Hemolysis |
|
Type III |
Immune |
IgG Multimers |
Soluble |
Complement, |
Serum Sickness |
|
Type IV |
Delayed-type |
CD4 T cell |
Soluble, |
Macrophage |
Contact Dermatitis (Ni+), PPD |
|
CD8 T cell |
Lipophilic |
Cytotoxicity |
Contact Dermatitis (poison ivy) |
Examples Of Haptens
And Hapten-Binding
Conjugates
There
are over 10k haptens, so here are the ones I think
are the most prominent/noteworthy:
·
Additives - Citric Acid,
Benzoates, Disulphides, Sulphates, Sulphur dioxide
and sulphites, aspartame, artificial
colors, MSG, disodium EDTA, xanthan gum R
·
Air Pollution R
·
Antibiotics - Beta-Lactams
(penicillin) R
·
Chemicals - Dinitrophenol,
formaldehyde, toluene diisocyanate, trimellitic
anhydride, phthalic anhydride, some benzene ring-containing compounds, ethylene
tetrachloride, ethylene oxide R
·
Drugs - Apresoline;
also Ipilimumab (anti-CTLA4), Pembrolizumab
(anti-PD-1) and Nivolumab (anti-PD-1) are used inhibit T cell immune-tolerant
states and can cause hapten-induced autoimmunity R
·
Dyes - Fluorescein; Red 1 and
6; in food, in hair coloring, etc R R
·
Estrogenics
- certain ones such as bisphenol-A (BPA), Octachlorostyrene
(from PVC) R R
·
Formula Milk as well
as casein and lactose R R
·
Fungal byproducts - e.g. those from Candida R R
·
Hormones - Digoxigenin; Estrogen R
·
Metals (esp
when oxidized)- Cobalt, Gold, Mercury, Nickel R R
·
Mycotoxins - Aflatoxin, Zeranol, Ochratoxin A R R R R
R
R
·
Nanoparticles/Nanomaterials
R R
·
Oxidized Fish Oil R
·
Pesticides, Insecticides, Fungicides, and
Organophosphates R
·
Plant Toxins - Urushiol (poison ivy),
Essential Oils (such as
cinnamaldehyde and tea tree), Thiocyanate
·
Sugar Alcohols -
Mannose intolerance seems to be common R R
·
Synthetic Peptides R
·
Toxins R
·
Vitamins - Biotin, fluorescein,
digoxigenin, and dinitrophenol R
·
VOCs - VOCs may also act as haptens by binding to endogenous proteins and sending
signals to activate immune system R R R
Fat
soluble haptens can get into cells easier.
Benefits Of Haptens
1. Cancer
Haptens may be
very beneficial for skin-related cancers. R R
Chemotherapy
drugs may synergize with folate-hapten–targeted
immunotherapy to reduce tumor growth. R
Haptens can
also be used to create certain cancer vaccines. R
2. Vaccines
Haptens can
create a higher IgG immune response, which may be beneficial for creating
effective vaccines. R R
Some
vaccines are being developed with haptens to combat
drug addictions (e.g. cocaine, opioids, nicotine etc) and food cravings (e.g. ghrelin-haptens)
as it may help cross the blood-brain barrier (BBB). R R R R
3. Hormone Signalling
Some hapten hormones have beneficial homeostatic properties,
such as Vitamin D and thyroid hormones (T3 and T4). R R
Symptoms Of Hapten
Sensitization
·
Aggression and Hyperactivity -
from swelling of the central nervous system (CNS) structures R
·
Atopic Dermatitis
(Eczema and Ichthyosis) - filaggrin barrier defects make it worse R R
R
·
Blood Pressure Drop - from
degranulation of a large number of mastocytes due to ionic disturbances R
·
Chemical Sensitivities and Environmental
Intolerance R
·
Drug-Induced Allergies (such
as those to antibiotics) R R R
·
Fatigue R
·
Feeling hot, even in cooler environments
(personal experience)
·
Histamine Problems
(and intolerance symptoms) R
·
Migraine Attacks - even
more prominent in children after consumption of chocolate, cocoa and sweets -
may be is explained by the low level of maturity of enzymatic systems in
children, reduced ability of binding compounds to plasma proteins, and the
ability of low-molecule compounds to penetrate a blood-brain barrier R
·
Skin hyperaemia
R
·
Tachycardia R
·
Urticaria - from destruction of
mastocytes and basophils R
Testing For Hapten
Sensitivity
Detection
of IgG and/or IgM antibodies against formaldehyde, trimellitic
anhydride, phthalic anhydride and benzene ring compounds is an indication of
chronic exposure to these chemical haptens. R
Based
on many case reports, if you have delayed hypersensitivity reactions, haptens may be the culprit. R R
Common
cytokines after chronic exposure:
·
Low (Th1):
o IFN-γ R
o IL-2, R
o IL-12 R
o TNFα R
·
High (Th2):
o IL-4 R
o IL-5 R
o IL-13 R
o IL-19 R
o IL-25 R
Haptens And Chemical Sensitivity
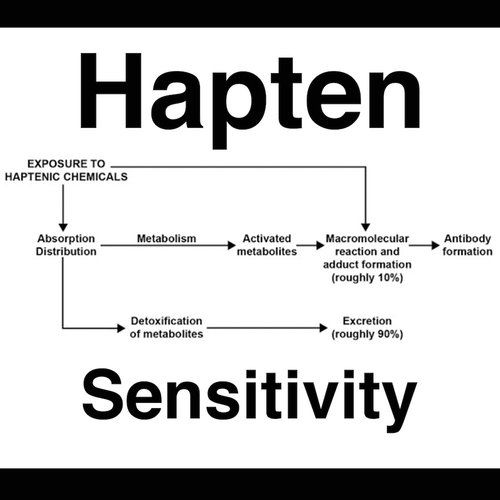
Usually,
haptens do not cause an immune response, and that may
be one reason why those without chemical sensitivities do not react from
chemicals. R
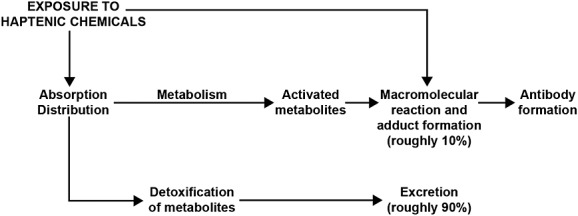
Haptens in
around 90% of the population get detoxed, and in the other 10%, haptens either bind to a protein to induce an immune
response or directly interact with the immune system creating antigens. R
Those
who are sensitive to haptens may be sensitive to
other small chemicals and have Chemical Sensitivities and/or Fragrance
(Perfume) Sensitivity.
Since haptens are so small they can get through the skin very
easily.
Haptens are
notorious for causing skin-induced contact sensitivity (sensitization) and is a
useful way to test for atopic dermatitis with chemicals and fragrances.
For
example, prehaptens from essential oils can auto-oxidize and become haptens, which then can cause sensitization of
the skin.
Haptens, Autoimmunity, And Food Intolerance
Haptens may
make you create antibodies towards your own self if they bind with your own
proteins (theory).
For
example, nicotine-based haptens are used to combat
addiction by creating anti-nicotine antibodies. R
1. Autoimmunity From
Drugs
Some haptens can induce autoimmune disease. R
For
example, hydralazine (blood pressure-lowering drug) can occasionally can
produce drug-induced lupus erythematosus in certain individuals. R
This
may be the mechanism by which the halothane (anesthetic) can cause
life-threatening hepatitis, as well as the mechanism by which penicillin-class
drugs cause autoimmune hemolytic anemia. R
2. Haptens,
Intestinal Permeability, And Food Intolerance
Case
reports have shown that the synergistic effect of multiple hapten
exposures with stress can to abnormal mucosal immune function and the breakdown
in immunological tolerance to dietary proteins and peptides. R
This
may be because when haptens bind to food proteins or
human tissue proteins, they can open tight junctions and elicit an immune
response.
For
example, after use of antibiotics (causing dysbiosis) or anesthetics, the
body may make antibodies to tight junctions in the gut, thus causing intestinal
permeability (leaky gut). R
Haptens can
also bind with food and human tissue, entering circulation and trigger an
autoimmune response. R
Haptens can
also bind to Lipopolysaccharides
(LPS) and create a greater antibody response. R R
The
ability for LPS bind with haptens and create
antibodies is more problematic with those with susceptible HLA or dysbiosis, and is less problematic in those
with immune tolerance (roughly 70-90% of the population). R
Having
increased intestinal permeability allows for the development of food
intolerances as well as other sensitivities (such as lectin sensitivity).
Haptens, Allergies, And Lectin Sensitivity
Haptens may
increase the risk of developing food IgE
(allergy) or IgG (intolerance) responses. R
Similar
to lectins, haptens are able to induce
allergic reactions directly because of their similarity to protein-bound sugar
(mannose). R
Haptens
directly compete with lectins for binding to glycans. R
Haptens can
also create complexes with lectins (such as the potato or pea hapten-lectin complex). R R
Dissimilar
to lectins, haptens do not use molecular mimicry but
bind to things that activate Toll-Like Receptors (TLRs, specifically
TLR2, TLR4, TLR6, and TLR9) and nucleotide-binding oligomerization domain
(NOD) like receptors (NLRs). R R R
In
those with celiac disease, the hapten complex of transglutaminase
2 (TG2) and gluten peptides by TG2-specific B cells may result in
activation of gluten-specific T cells which subsequently provide help for the B
cells to secrete autoantibodies. R
Haptens After Tregs Loss
Haptens are a
very common driver of problems after infections (such as Lyme, CIRS, mold, dysbiosis, candida, etc). R
For
example, aflatoxin (mycotoxin) is a known hapten
that binds to human tissue, causing an autoimmune response. R
Haptens may be
part of the reason why some people can be both Th1 and Th17, but
over time may become more Th2 dominant (as well as have histamine intolerance
and/or mast cell problems) via the "danger
limitation effect". R
Haptens also
can increase Suppressor of Cytokine Signalling 3 (SOCS3)
expression, thus promoting more Th2 dominance (especially in the skin). R R
Losing Tregs
makes all of this worse and can help predispose you to hapten
sensitivity. R
Other Harms Of Haptens
·
Alcohol Intolerance -
Those that are sensitive to haptens may have adverse
allergic-like reactions to alcohol. It has been shown that individuals with
severe hypersensitivity reactions to ethanol have elevated levels of
circulating anti-acetaldehyde– protein IgE
antibodies... In these studies, the acetaldehyde moiety has been shown to be
acting as a hapten. R
·
Anhedonia and Depression -
possibly through TLR4 activation and LPS binding R
·
Antibiotic-induced allergy R R R R R R R
·
Arthritis R
·
Autism Spectrum Disorders - the
immunotoxins causes “activation” of the immune system
leading to the production of autoantibodies against haptens
R
·
Cancer R
·
Change in neurotransmission (via Mannich reaction) - haptens can
be made to bind to neurotransmitters and biogenic amines such as tryptamine,
serotonin, 5‐hydroxy‐indole acetic acid
(5-HIAA), melatonin, tyramine, dopamine,
dihydroxyphenyl acetic acid (DOPAC), norepinephrine, glycine, glutamate,
glutamine, and GABA. R
·
Dampened Immune System - Haptens may also block immune responses through "hapten inhibition" and cause the immune system not to
respond to foreign invaders. R
·
Decreased Sun Protection from UV
(in those genetically predisposed) R
·
Disrupts good biofilms of the
microbiome R
·
Inflammatory Bowel Disease (IBD) R
·
Liver Failure R
·
Vision Loss - Haptens
generated from oxidized DHA can cause age-related macular degeneration
(AMD) R
·
Vitiligo -
from the destruction of melanocytes R
What To Do If You Are Sensitive To Haptens
Avoidance And Regulation
1.
Avoid Exposure -
Avoid all exposure to unnecessary haptens and
properly handle chemicals (no megadoses or prolonged
exposure).
2.
Binding and Chelation -
depending on the type of hapten, it may be necessary
to bind/chelate it - e.g. mercury
3.
Dysbiosis - Avoid
anything that can induce dysbiosis, such
as antibiotics, glyphosate, etc, as they can open up tight junctions allowing for LPS +
haptens to create autoimmunity and food intolerance. R
4.
Immune Tolerance -
Avoid factors that can decrease immune tolerance as those with immune tolerance
are significantly less likely to developing sensitivity to haptens.
R R
5.
Proper redox - NRF2 dysfunction can allow haptens to cause problems with antioxidant status. R R
Fixes
·
alpha-Melanocyte-stimulating
hormone (alpha-MSH) - can induce hapten-specific
tolerance (in skin) R
·
Antihistamines (Histamine
H1 + H4 receptor antagonists) - helps with hapten-induced
scratching and inflammation R
·
Astragalus -
protects against hapten-induced colitis. R
·
Bitter Leaf
(Vernonia amygdalina) - prevent and improve atopic/eczema dermatitis syndrome R
·
Chitosan
(chitin)- helps with lectin-LPS-hapten binding R
·
Dietary Indoles such
as I3C and DIM - may help
increase immunotolerance to haptens R
·
Glutathione -
reduces inflammation in sensitized skin R
·
H2S therapy - reduces inflammation,
restores the microbial biofilm, and increases the production of mucus granules R
·
IGF-1 - reduces hapten-induced inflammation R
·
Increase IL-10 R
·
Increase Tregs - hapten sensitivity is highly dependent on
regulatory t-cell status R
·
Lactobacillus casei - exerts protective effects on T
cell–mediated skin inflammation by increases in FoxP3+ Tregs R
·
LXR activation R
·
PPARα
activation R
·
PXR activation R
·
Topical Corticoids R
·
Vasoactive Intestinal Polypeptide (VIP)
- helps with hapten induced arthritis and colitis R
Genes That Make You More Susceptible To Haptenation
...will
come back to this soon with more SNP information if possible.
DNFB
Soluble
factors in tolerance and contact sensitivity to 2,4-dinitrofluorobenzene in
mice. III. Histocompatibility antigens associated with the hapten
dinitrophenol serve as target molecules on 2,4-dinitrofluorobenzene-immune T
cells for soluble suppressor factor. R
Induction
of tolerance to 1-fluoro-2,4-dinitrobenzene contact sensitivity with hapten-modified lymphoid cells. II. Selective tolerance in
F1 mice of T cell subsets recognizing 1-fluoro-2,4-dinitrobenzene associated
with parental major histocompatibility complex antigens. R
H-2
restriction of suppressor T-cell induction by hapten-modified
lymphoid cells in tolerance to 1-fluoro-2,4-dinitrobenzene contact
sensitization. R
HNOX-1 (heme nitric oxide/oxygen)
NQa1
SLIT2
Expression
of Slit2 in skin has been reported to be upregulated at both 4
hours and 48 hours following hapten sensitization,
suggesting Slit2 can have a role both early and late in an
inflammatory response. R
Other Mechanisms Of
Haptens
Simple:
·
Increases B Defensins R
·
Increases CCL1 R
·
Increases CCL5 R
·
Increases CXCL2 R
·
Increases CXCL-10 R
·
Increases C5a R
·
Increases E-selectin R
·
Increases Fibrinogen R
·
Increases FnEDA+ R
·
Increases GM-CSF R
·
Increases Heparin Sulfate R
·
Increases ICAM-1 R
·
Increases IFNγ
R
·
Increases IgM R
·
Increases IL-1β R
·
Increases IL-4 R
·
Increases IL-17 R
·
Increases IL-18 R
·
Increases NLRP3 R
·
Increases PGE2 R
·
Increases P-selectin R
·
Increases ROS R
·
Increases Serotonin R
·
Increases Tenascin R
·
Increases TLR2 R
·
Increases TLR4 R
·
Increases TLR6 R
·
Increases TLR9 R
·
Increases TNFα R
^most
of these are from acute exposure
Advanced:
·
Early on
o γδ-T cells can recognize haptens and mount a hapten-specific
immune response stimulated release of IL-17. R
·
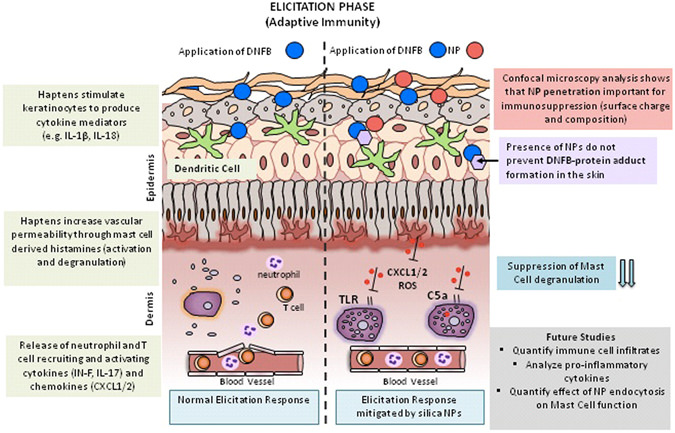
Contact hypersensitivity
o Sensitization - Hapten application induces strong innate immune mechanisms,
causing cell death and the release of danger signals and endogenous ligands,
leading to cytokine release, IL-1β,
IL-18, TNFα, and GM-CSF, by keratinocytes (KC). This release will stimulate
dermal antigen-presenting cells (dAPCs), langerhans cells, and dermal dendritic cells, to take up haptenated antigen and migrate to the dLN
to activate naïve T-cells. Mast cells will aid in this migration by releasing
TNFα. iNKT cells in the liver will be
activated by APCs presenting haptenated glycolipid by
CD1d. This will cause cytokine release, IL-4, to stimulate naïve B-1 cells in
the peritoneal cavity, along with the binding of hapten-antigen
by membrane IgM. This will cause migration of these cells to the dLN, and subsequent maturation into CS-initiating B-1
cells, which release antihapten IgM into circulation.
R
o Early
phase - Hapten challenge will
restimulate iNKT cells to release IL-4, which along
with hapten-antigen will stimulate CS-initiating B-1
cells. These cells will release IgM, which will bind to hapten-antigen.
This will cause formation of C5a, triggering activation of mast cells to
produce TNFα and serotonin, increasing immune cell trafficking into the area
and TNFα and CXCL2 to stimulate neutrophils in the dermis R
·
Drug-induced hypersensitivity
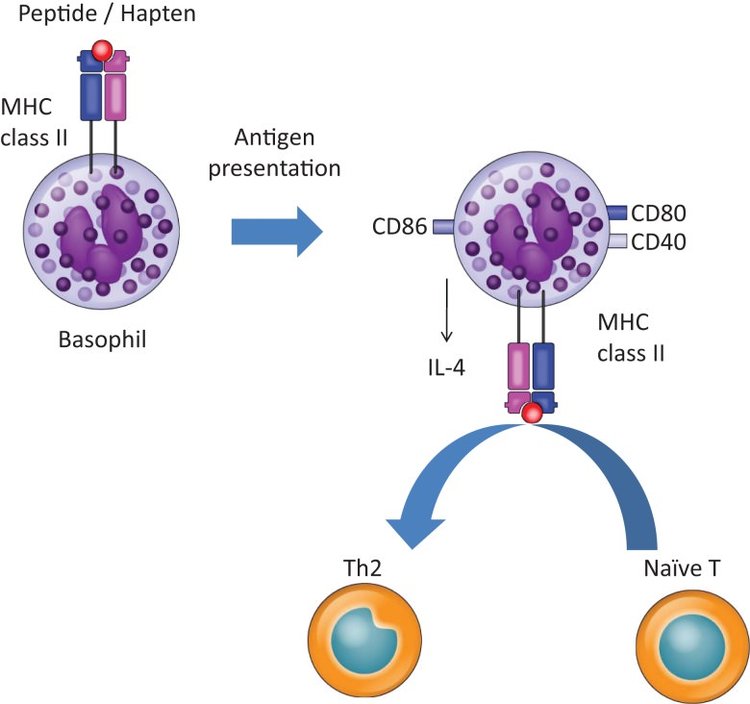
o Most
drugs are small molecules and are by themselves, not immunogenic. During the
haptenization process, these small molecules bind to carrier proteins to form a
complete immunogenic complex. The hypersensitivity reaction then requires the
activation and maturation of dendritic cells (DCs), which will then drive the
activation of specific T cells. DCs are antigen-presenting cells (APC) that
play a central role in the initiation and regulation of adaptive immune
responses. Following the contact with antigens, DCs undergo a process of
maturation associated with the expression of several co-stimulatory molecules
on the membrane such as CD80, CD86 and CD40, various adhesion molecules (CD2,
CD11a, CD54, CD58), and secrete different cytokines, including IL-1β and
IL-8. Once activated, DCs migrate into the regional lymph node or in the
spleen, where they present antigen to specific T lymphocytes, through MHC class
II molecules and co-stimulatory adhesion molecules expressed on both DC (i.e.,
CD86) and T cell (i.e., CD28) to ensure the necessary contact to achieve full T-cell
activation. Following stimulation, a clone of T cells is produce
with the ability to react to the antigen, resulting in the clinical
manifestation of HDR. R
·
Prohaptens and Prehaptens
o Prohaptens are chemicals that are
not protein reactive unless they are metabolically activated to electrophilic
species. It has also been proposed that prohapten
chemicals that undergo air oxidation to reactive species be classified
separately as prehaptens, but the criteria on when a
chemical is a pro- or prehapten is
confusing...Bioactivation of prohaptens commonly
involves oxidative processes, with the cytochrome P450 system (CYPs) playing a
major role in the biotransformation of the majority of prohaptens
to sensitizers. CYP enzymes that have been detected at the mRNA level in the
skin include CYP1A1, 1B1, 2B6, 2E1, and 3A5...Once bioactivated to an
electrophilic species, haptenation of proteins
proceeds via one of the previously discussed mechanisms. R R
·
Microbiome and Bile regulation
o Secondary
bile acids, such as DCA and LCA, regulate the immune system, in part, through
their receptors, such as TGR5 (also called GPBAR1 or M-BAR) and two nuclear
receptors, FXR and PXR. Animals deficient in TGR5 develop more severe colitis
induced by T cell-activating haptens (TNBS and
oxazolone). R
·
Haptens and
Redox Status
o The majority of occupationally related haptens are reactive, electrophilic chemicals, or are metabolized to reactive metabolites that form covalent bonds with nucleophilic centers on proteins. Nonelectrophilic protein binding may occur through disulfide exchange, coordinate covalent binding onto metal ions on metalloproteins or of metal allergens, themselves, to the major histocompatibility complex. Recent chemical reactivity kinetic studies suggest that the rate of protein binding is a major determinant of allergenic potency; however, electrophilic strength does not seem to predict the ability of a hapten to skew the response between Th1 and Th2. R